Canadian Stats on Rates 2025
- While some types of cancer (lung/colorectal) are on a decline, oral cancer may be increasing in some demographics
- After being on a downward trend for over 20 years, oral cancers increased by 3.4% per year between 2003 and 2013, largely due to HPV infections
- Over 8000 new head/neck/oral cancers with over 2000 deaths per year in 2025.
- Men are affected more than women at a ratio of 2:1
- Most common in those over 45
- The 5-year survival for oral cancers is 64% and is greatly affected by early vs late diagnosis
- Overall cancer mortality in Canada is decreasing; however, the number of new cases has been increasing due to the aging population
- Oropharyngeal cancers (back of throat, tonsils, tongue base) linked to Human Papilloma Virus (HPV) infection are on the rise
- HPV is the most common sexually transmitted infection, with nearly all sexually active individuals contracting it at some point in their lives
- Generally, HPV infections come and go within 1-2 years; however, HPV that remains is what can lead to cancer.
- In Canada, about 2/3 of HPV-related cancers happen in areas other than the cervix
- HPV is spread primarily through skin-to-mucosa contact
5-Year Relative Survival By Stage & Tumour Site
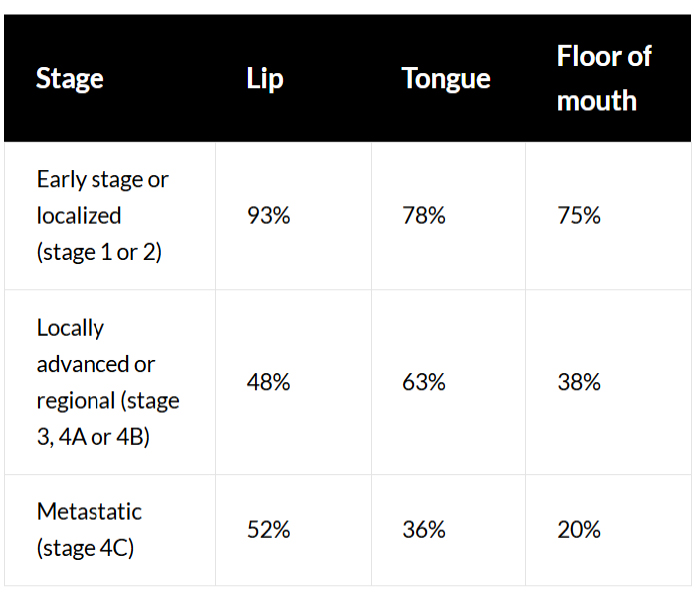
When to Act
See your dentist or medical doctor if you notice the following symptoms that persist for more than 10-14 days.
What to Look For
- White or red/ulcerated lesion with unknown cause that does not heal within 14 days.
- Difficulty swallowing, chewing, speaking, or moving the tongue
- Persistent ear pain
- Persistent sore throat, hoarseness, or feeling that something is caught in the throat
- Changes to taste or tongue sensation
- Lumps on the tongue, face, or neck
- Numbness or tenderness in the mouth with no known cause
Infections
- A weakened immune system due to cancer treatment makes patients more susceptible to infections caused by bacteria, fungi (thrush), or viruses (herpes).
- Antimicrobial therapy to treat the infection can harm gut bacteria.
- The timing of antimicrobials relative to immunotherapy is critical.
- Don't take antibiotics for viral infections (like colds) or if a doctor hasn't confirmed a bacterial infection.
Tooth & Gum Problems
- The combination of dry mouth, changes in mouth bacteria, and discomfort from cancer therapy increases the risk of tooth decay and gum disease.
- Lowered platelet levels in the blood can lead to difficulty with blood clotting and, therefore, bleeding gums.

Risk Factors
Age: Those over age 45 and especially older than 60 have the highest incidence of oral cancer
Smoking: Any tobacco product increases the risk of oral cancer, especially when combined with high alcohol consumption
Alcohol: Increases in alcohol consumption and the length of time used increase oral cancer risk
Gender: Men are more susceptible than women
Diet: Low consumption of fruits and vegetables decreases important micronutrients and antioxidants that protect against cancers
Poor oral health
Sun exposure: risk is increased further for those who do not use sun protection
Family hx of oral cancer: Especially when combined with other risk factors
Ill-fitting dentures: May create sores in the mouth that trap carcinogens such as alcohol and tobacco
HPV: The prevalence of oropharyngeal cancers due to HPV infection rose form 47% in 2000 to 74% in 2012
What Should Your Dentist Or Oral Health Care Provider Be Doing
1. Prevention
Getting the HPV vaccine helps to protect against HPV infections and reduce the risk of oropharyngeal cancer. There are more than 200 types of HPV so even if you have been infected with HPV in the past, getting the vaccine now can help protect you from the types of HPV which you have not been exposed to.
- Maintain good oral hygiene habits, such as brushing the teeth daily
- Minimize prolonged sun exposure by wearing sunscreen and/or UV protective clothing
- Use a condom when sexually active
- Eat a variety of healthy foods daily, including vegetables and fruits
- Quit or reduce tobacco and alcohol consumption
- See an oral health professional to adjust ill-fitting dentures
HPV Vaccinations
Cervarix: This vaccine protects females aged 9 to 45 against HPV types 16 and 18. Because Cervarix protects against 2 types of infection, it's called a bivalent vaccine. Cervarix doesn't protect against genital warts.
Gardasil 9: Gardasil 9 protects people aged 9 to 45 against 2 types of HPV that cause genital warts and 7 types of HPV that cause cancer, including types 16 and 18. Because Gardasil 9 protects against 9 types of infection, it's called a nonavalent vaccine.
2. Screening
See an oral health professional a minimum of twice yearly
Perform self-examination regularly by feeling your neck, jaw, and intraoral tissues for lumps and changes
Early detection is key and improves the chances of successfully treating oral cancer. There will be less likelihood of the cancer cells spreading to other parts of the body
When caught early, 5-year cancer survival rates range from 80-95%
If cancer has spread to surrounding tissues, the 5-year survival rate drops to 68% or lower
3. Oral Cancer Exam at Your Dental Office
Your dentist or dental hygienist can perform the exam at least twice per year.
This includes:
Updating health history for signs of difficulty swallowing or opening the jaw
Counselling on sun protection
Feel your neck, jaw, face, and the back of the head
Stretch the lips and cheeks for better visualization
Stretch the tongue to view the sides of the tongue and the floor of the mouth
Examine the gums and the roof of the mouth
Use oral cancer detection lights to look for any abnormalities
Common Oral Cancer Myths
- Only smokers and drinkers develop oral cancer - The risk is higher if you drink and/or smoke, but 25% of oral cancers occur in those who don't smoke or drink
- Only older adults should be screened - the incidence of oral cancer is most prevalent in those over 60; however, rates in younger individuals are on the rise
- The incidence of oral cancer is lower than certain other cancers, while it is not the most common type of cancer, the rate of oral cancer is 3 times higher than cervical cancer and double that of liver cancer
- Oral health is irrelevant - the incidence of oral cancer has been linked to periodontal disease in a study from the National Library of Medicine
If An Abnormality Is Detected
- Your dentist will refer you to a specialist, such as an oral pathologist or oral surgeon.
- The specialist will discuss your options and, generally, take a biopsy of the lesion.
- The results of the biopsy take 2-6 weeks to be returned to the specialist's office, at which time you will have a follow-up appointment.
- If the results are negative, you may be followed on an annual basis to ensure that no further lesion develops.
- If the results are positive, you will be referred to Cancer Care Manitoba to discuss treatment options with an oncologist.
What to Expect If You Have Oral Cancer Treatment
- Dry mouth
- Inflammation of the oral tissues
- Taste changes or complete loss of taste
- Higher risk of tooth decay
- Decreased immune system
- Bleeding gums
- Osteoradionecrosis (bone death) from radiation to the head/neck
- Stiffness of the jaw
What To Do Before Treatment Begins
- Visit your dentist to assess the health of your mouth
- Have your teeth cleaned to create a healthy baseline
- Find oral products that will be helpful during cancer treatment
- Ask for help! Allow friends and family to help with meals and transportation
What To Do During Treatment
- Notify your dental team about signs or symptoms
- Gentle brushing and rinsing with non-alcohol-containing products
- Avoid spicy, acidic, or hard foods; choose softer options
- Stay hydrated by sipping water often
- Use fluoride trays from your health care provider to protect your teeth
- Moisturize lips with a water- or plant-based lip balm. Avoid petroleum products, as they will trap bacteria
- Gentle exercise, massage, or heat therapy for jaw stiffness
What To Do After Treatment
- Visit your dentist regularly to monitor any long-term oral side effects and to screen for recurrence
- Continue using products for dry mouth as needed
- Manage anxiety from diagnosis and treatment by practicing relaxation and mindfulness
- Prioritize sleep and a healthy diet
- Regular physical activity
Patients Who Are in Remission or Cured Should Be Recommended an Oral Recall Program
First 2 years following treatment: 1-3 month recall
2-5 years: 3-6 months recall
5 years: minimum of once/year
